Nephrotic Syndrome | Vibepedia
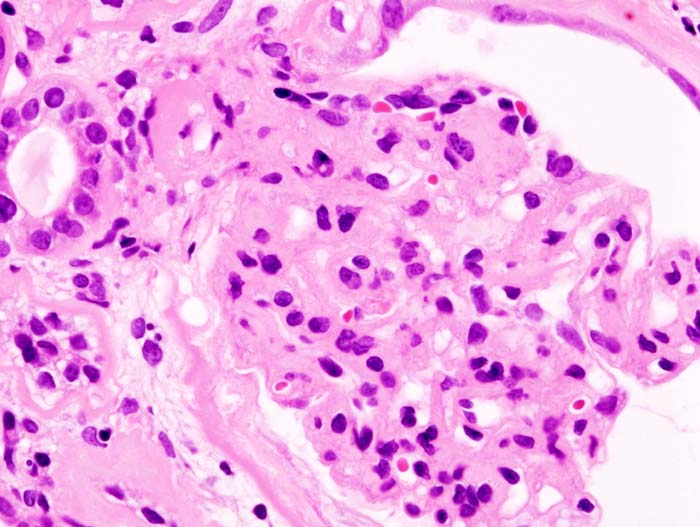
Nephrotic syndrome isn't a singular diagnosis but rather a clinical presentation arising from significant kidney damage, specifically affecting the glomeruli…
Contents
Overview
Nephrotic syndrome isn't a singular diagnosis but rather a clinical presentation arising from significant kidney damage, specifically affecting the glomeruli. It's characterized by a quartet of hallmark symptoms: proteinuria (excess protein in the urine), hypoalbuminemia (low blood albumin levels), hyperlipidemia (high blood lipid levels), and edema (significant swelling). This cascade of effects can lead to secondary issues like weight gain, fatigue, foamy urine, and potentially life-threatening complications such as blood clots, infections, and hypertension. While often stemming from primary glomerular diseases like FSGS or minimal change disease, it can also be a consequence of systemic conditions like diabetes, lupus, or amyloidosis. Diagnosis hinges on urine analysis and often requires a kidney biopsy, distinguishing it from its close relative, nephritic syndrome, by the absence of significant red blood cells in the urine. Treatment is a complex dance, focusing on eradicating the root cause while managing the symptomatic fallout, often involving dietary modifications and medications to control blood pressure and cholesterol.
🎵 Origins & History
The understanding of nephrotic syndrome has evolved significantly since its initial descriptions in the late 19th and early 20th centuries. Early observations noted the characteristic edema and albuminuria, laying the groundwork for recognizing it as a distinct clinical entity. The term 'nephrotic syndrome' itself gained traction as the understanding of glomerular pathology deepened. The identification of specific underlying causes, such as lipoid nephrosis (now known as minimal change disease) and later work in the mid-20th century, began to differentiate the syndrome from a monolithic disease. The advent of kidney biopsy in the mid-20th century provided crucial histological insights, allowing for more precise diagnoses and targeted treatments, moving beyond purely symptomatic management.
⚙️ How It Works
Nephrotic syndrome manifests when the glomerular filtration barrier in the kidneys is compromised, leading to excessive leakage of protein, primarily albumin, from the blood into the urine. This protein loss, known as proteinuria, is the central driver of the syndrome's other features. As albumin levels in the bloodstream drop (hypoalbuminemia), the oncotic pressure decreases, causing fluid to shift from the blood vessels into the interstitial tissues, resulting in widespread edema. Simultaneously, the liver attempts to compensate for the protein loss by increasing lipid synthesis, leading to hyperlipidemia, characterized by elevated levels of cholesterol and triglycerides. The damaged glomeruli also impair the kidney's ability to filter waste products and regulate fluid balance, contributing to potential complications like high blood pressure and electrolyte imbalances. The specific insult to the glomeruli can range from immune-mediated damage in minimal change disease and membranous nephropathy to structural changes in FSGS or systemic diseases like diabetes.
📊 Key Facts & Numbers
Globally, nephrotic syndrome affects individuals with varying prevalence across different age groups and ethnicities. In children, minimal change disease is a common cause, with a high remission rate with steroid treatment. For adults, FSGS and membranous nephropathy are more common primary causes, often requiring more aggressive immunosuppressive therapy and carrying a higher risk of progression to kidney failure. Some cases are secondary to systemic diseases like diabetes or lupus. The risk of developing blood clots (thromboembolism) is significantly elevated, particularly with severe hypoalbuminemia below 2.0 g/dL. Some adults with primary nephrotic syndrome will eventually require kidney transplantation or dialysis.
👥 Key People & Organizations
Key figures in understanding nephrotic syndrome include Sir William Gull, who first described the clinical features. Later, Frank McCombs Childs identified minimal change disease, a crucial step in classifying causes. The National Kidney Foundation and the KDIGO initiative play vital roles in establishing clinical guidelines and promoting research. Organizations like the Nephrotic Syndrome Foundation and Kidney Research UK fund research and support patients. Leading research institutions such as Boston Children's Hospital and Mayo Clinic are at the forefront of investigating new therapeutic strategies and understanding the molecular mechanisms underlying glomerular damage.
🌍 Cultural Impact & Influence
Nephrotic syndrome, while a medical condition, has permeated cultural understanding through its impact on individuals and families, often highlighting the challenges of chronic illness. Public awareness campaigns, often spearheaded by patient advocacy groups like the Nephrotic Syndrome Foundation, aim to destigmatize kidney diseases and promote early detection. The narrative of battling chronic conditions, including nephrotic syndrome, has been featured in various forms of media, from documentaries to personal memoirs, fostering empathy and understanding. The visual representation of edema, a prominent symptom, can be a stark reminder of the body's internal struggles. Furthermore, the economic burden of managing chronic kidney disease, including nephrotic syndrome, influences healthcare policy discussions and resource allocation, impacting societal priorities.
⚡ Current State & Latest Developments
Current research is intensely focused on developing targeted therapies that go beyond broad immunosuppression. Advances in genetics are identifying specific gene mutations linked to primary forms of nephrotic syndrome, such as NPHS1 and NPHS2, paving the way for potential gene therapies or precision medicine approaches. The development of novel drugs targeting specific pathways involved in podocyte injury and proteinuria, such as endothelin receptor antagonists and SGLT2 inhibitors, shows promise in clinical trials. For steroid-resistant nephrotic syndrome, the use of calcineurin inhibitors like cyclosporine and tacrolimus remains a cornerstone, but research into more effective and less toxic alternatives is ongoing. The role of the gut microbiome in modulating immune responses and inflammation in nephrotic syndrome is also an emerging area of investigation.
🤔 Controversies & Debates
A significant debate revolves around the optimal duration and intensity of immunosuppressive therapy, particularly for steroid-sensitive nephrotic syndrome in children, to minimize long-term side effects like growth stunting and osteoporosis. The precise definition and management of 'focal segmental glomerulosclerosis' (FSGS) itself remain contentious, with ongoing discussion about whether it represents a single entity or a final common pathway for various insults. Furthermore, the balance between aggressive treatment to achieve remission and the potential toxicity of medications is a constant challenge, especially in vulnerable populations. The increasing recognition of genetic causes is also prompting discussions about the role of genetic screening in diagnosing and managing familial forms of nephrotic syndrome.
🔮 Future Outlook & Predictions
The future of nephrotic syndrome management likely lies in personalized medicine, driven by advances in genomics and biomarker discovery. Identifying specific genetic predispositions and molecular signatures of disease will enable tailored treatment strategies, moving away from a one-size-fits-all approach. The development of regenerative medicine techniques, such as stem cell therapy aimed at repairing damaged podocytes, holds long-term potential. Furthermore, a greater understanding of the interplay between the immune system, genetics, and environmental factors will likely lead to novel preventative strategies. The goal is to not only achieve remission but also to prevent disease recurrence, preserve kidney function long-term, and improve the overall quality of life for affected individuals, potentially reducing the reliance on dialysis
Key Facts
- Category
- science
- Type
- topic