Influenza | Vibepedia
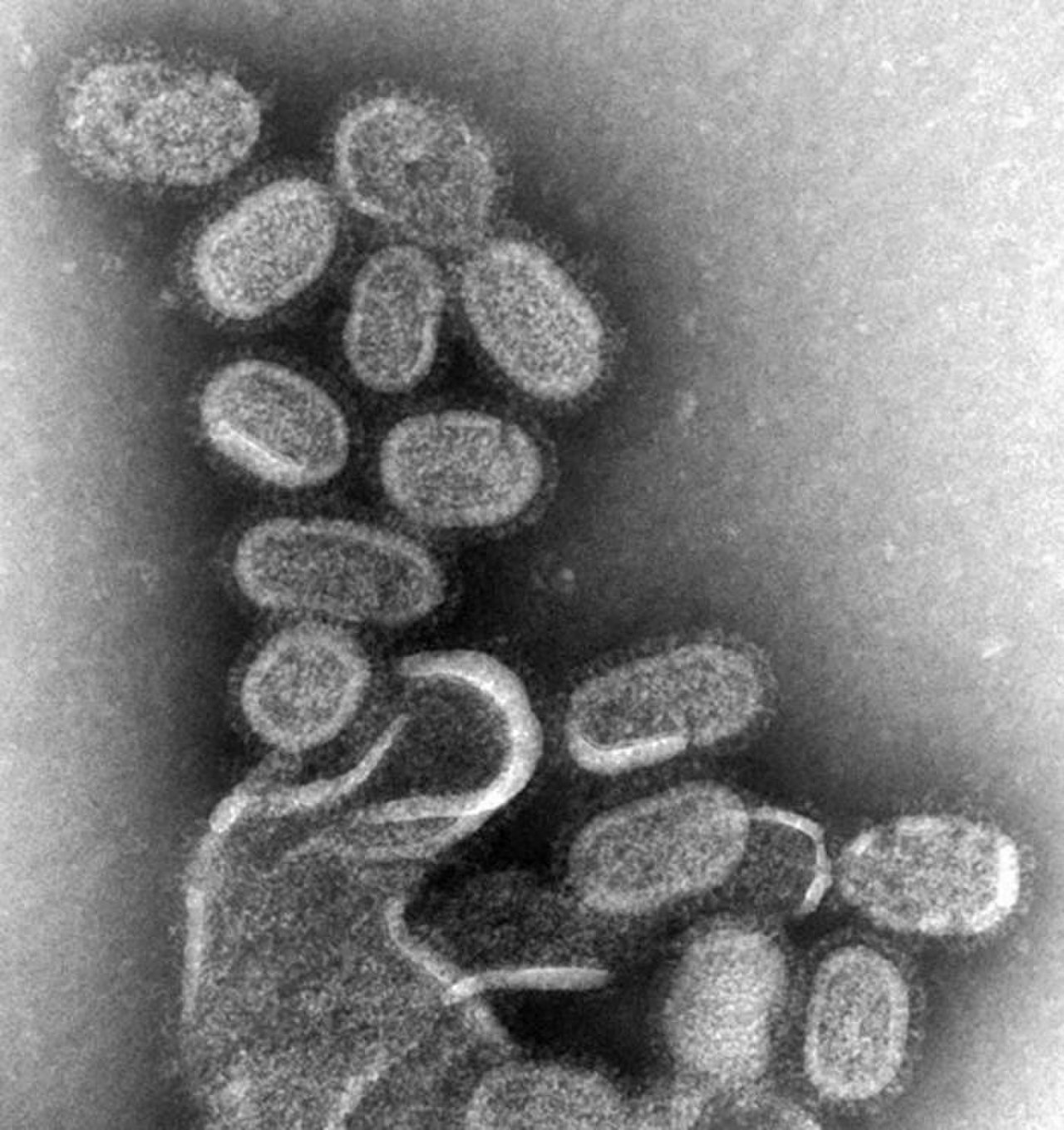
Influenza is not a 'bad cold'; it is a sophisticated molecular machine defined by the constant reshuffling of Hemagglutinin (H) and Neuraminidase (N) surface…
Contents
Overview
Influenza is not a 'bad cold'; it is a sophisticated molecular machine defined by the constant reshuffling of Hemagglutinin (H) and Neuraminidase (N) surface proteins. While the 1918 H1N1 pandemic remains the historical benchmark with an estimated 50 million deaths, the modern threat lies in the 'antigenic shift'—sudden genetic reassortments often originating in avian or swine reservoirs that bypass human immune memory. The global surveillance apparatus, led by the WHO’s GISRS network, attempts to predict dominant strains months in advance for vaccine production, a process that remains a high-stakes gamble against viral evolution. Beyond the biology, influenza dictates global labor productivity, pharmaceutical supply chains, and the structural integrity of healthcare systems every winter. It is the only recurring global event that forces a total recalibration of international public health policy on an annual basis.
🦠 What is Influenza?
Influenza, or the flu, is a highly contagious respiratory illness caused by influenza viruses. It's not just a bad cold; it's a distinct pathogen that can sweep through populations with alarming speed. Symptoms typically manifest 1-4 days post-exposure, presenting as fever, cough, sore throat, muscle aches, headache, and profound fatigue. While often self-limiting, influenza can lead to severe outcomes, particularly for vulnerable groups. Understanding its transmission and impact is crucial for navigating public health challenges.
📈 Global Impact & Vibe Score
Globally, influenza is a persistent public health concern, responsible for an estimated 290,000 to 650,000 respiratory deaths annually, according to the WHO. Its Vibe Score, measuring cultural energy and societal impact, hovers around 75/100, reflecting its constant presence in public discourse and healthcare systems. The economic burden is substantial, with lost productivity and healthcare costs running into billions of dollars each year. This recurring threat necessitates continuous vigilance and adaptation in our biosecurity measures.
🔬 The Science: How it Works
The influenza virus, belonging to the Orthomyxoviridae family, is an RNA virus with segmented genomes. This segmentation is key to its evolutionary agility, allowing for rapid genetic reassignment (reassortment) when different strains co-infect a host. The virus primarily infects cells in the respiratory tract, hijacking cellular machinery to replicate. Its surface proteins, hemagglutinin (HA) and neuraminidase (NA), are critical for viral entry and release, and are the primary targets for the immune system and vaccine development. Understanding these molecular mechanisms is fundamental to combating the virus.
💡 Historical Context & Evolution
The history of influenza is punctuated by devastating pandemics. The 1918 Spanish Flu pandemic, caused by an H1N1 strain, is estimated to have killed 50-100 million people worldwide, a staggering figure that reshaped global demographics and public health infrastructure. Subsequent pandemics, like the 1957 Asian Flu (H2N2) and the 1968 Hong Kong Flu (H3N2), and the 2009 Swine Flu (H1N1pdm09), demonstrate the virus's persistent capacity for global disruption. Each outbreak has informed our understanding of viral evolution and pandemic preparedness.
💉 Prevention & Mitigation Strategies
Preventing influenza hinges on a multi-pronged approach. Annual vaccination remains the cornerstone of defense, with vaccines typically targeting the most prevalent strains predicted by the WHO and the CDC. Beyond vaccination, good hygiene practices—frequent handwashing, covering coughs and sneezes—are vital in limiting transmission. Antiviral medications, such as oseltamivir (Tamiflu), can reduce the severity and duration of illness when administered early. Public health campaigns play a critical role in promoting these preventive behaviors.
⚠️ Complications & Risks
While many influenza infections resolve without incident, complications can arise, transforming a mild illness into a life-threatening condition. These include secondary bacterial pneumonia, which can be particularly severe, and viral pneumonia. Neurological complications like encephalitis (brain inflammation) and meningitis, as well as exacerbations of chronic conditions such as asthma and heart disease, are also documented risks. Acute respiratory distress syndrome (ARDS) is a severe, potentially fatal outcome requiring intensive medical intervention.
🤔 Debates & Controversies
The influenza landscape is marked by ongoing debates, particularly concerning vaccine efficacy and mandates. Questions arise about the optimal timing for vaccine production and distribution, given the virus's rapid mutation rate. There's also discussion around the balance between individual liberty and public health imperatives regarding vaccination policies. Furthermore, the effectiveness and accessibility of antiviral treatments, especially in resource-limited settings, remain points of contention. The development of universal flu vaccines, targeting conserved viral regions, is a major area of research and debate.
🔮 Future Outlook & Biosecurity
The future of influenza management is intrinsically linked to advancements in biosecurity and surveillance. Enhanced global surveillance networks are crucial for early detection of novel strains with pandemic potential. The development of next-generation vaccines, including universal flu vaccines, promises more durable and broad-spectrum protection. Investment in rapid diagnostic tools and robust public health infrastructure will be essential to mitigate the impact of future outbreaks. The ongoing arms race between viral evolution and human intervention defines the future of influenza control.
Key Facts
- Year
- 1933
- Origin
- London (First isolation of human influenza virus by Smith, Andrewes, and Laidlaw)
- Category
- Pathology & Biosecurity
- Type
- Viral Pathogen
Frequently Asked Questions
How is influenza different from the common cold?
Influenza is generally more severe than the common cold, with symptoms that appear more suddenly and intensely. While colds primarily affect the nose and throat, the flu often causes fever, body aches, and extreme fatigue that can last for weeks. Influenza also carries a higher risk of serious complications like pneumonia.
Who is most at risk for severe influenza complications?
Individuals at highest risk include young children, pregnant women, people aged 65 and older, and those with chronic medical conditions such as asthma, diabetes, heart disease, and compromised immune systems. These groups are more likely to experience severe illness and require hospitalization.
How often should I get a flu shot?
The CDC recommends annual influenza vaccination for everyone six months of age and older. Because flu viruses change each year, and immunity from vaccination wanes over time, an updated vaccine is needed annually to provide optimal protection.
Can I get the flu from the flu shot?
No, the flu shot cannot give you the flu. Most flu shots are made with inactivated (killed) virus or with only a single gene from the virus. The nasal spray flu vaccine contains live but weakened viruses that do not cause illness in healthy people. Some people may experience mild side effects like soreness at the injection site, a low-grade fever, or muscle aches, which are signs of the immune system building protection.
What are the signs of a severe flu infection that require immediate medical attention?
Seek emergency care if you experience difficulty breathing or shortness of breath, pain or pressure in the chest or abdomen, sudden dizziness, confusion, severe or persistent vomiting, or if flu-like symptoms improve but then return with fever and worse cough. In children, emergency warning signs include fast breathing or trouble breathing, bluish skin color, not drinking enough fluids, not waking up or interacting, being so irritable that the child does not want to be held, or fever with a rash.
How long is someone with influenza contagious?
People with influenza are typically most contagious during the first 3-4 days of their illness. However, they can spread the virus to others from 1 day before they develop symptoms to about 5-7 days after becoming sick. Some people, especially young children and those with weakened immune systems, may be contagious for longer periods.